A growing body of research suggests oestrogen levels throughout a woman’s life may influence her risk of developing Alzheimer’s disease. In this case, more oestrogen appears to be better.
Alzheimer’s disease is one of the leading causes of death in Australia and is increasing in incidence. Those suffering from Alzheimer’s experience intense isolation and depression, and long-term care is dramatically more expensive than other common serious conditions. Although there are available medications for treatment of Alzheimer’s, prevention or cure of the disease remains elusive.
When researchers have looked into health histories of large groups of women, an interesting pattern appears. Life events demonstrate that greater exposure to oestrogen throughout a woman’s life may be linked to a decrease in Alzheimer’s. Events such as when she starts her first menstrual cycle (earlier is better), how many pregnancies she has (more are better) and how late she goes into menopause (later is better) can affect a woman’s risk. These findings have led researchers to explore the potential benefits of oestrogen therapy for lowering Alzheimer’s risk. However, early in life menstrual cycles and late menopause increase a woman’s risk for breast cancer, so caution should be used when assessing the appropriateness of hormone therapy.
Currently oestrogen replacement therapy is not recommended for prevention of Alzheimer’s disease. However, a study looking at deceased females found that those who used oestrogen for menopause symptoms were significantly less likely to have had a diagnosis of dementia or Alzheimer’s. More convincingly, in those who used higher doses of oestrogen for longer periods, the benefit was more pronounced. Women who start oestrogen replacement therapy more than 10 years after the onset of menopause had no benefit, which indicates that oestrogen deprivation for several years may have irreversible impact on brain health.
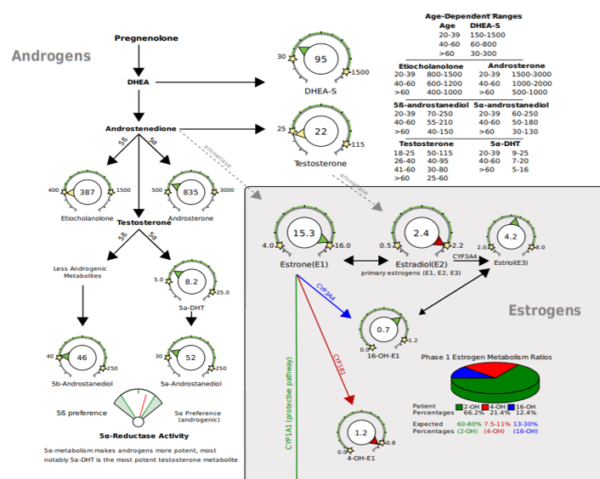
The most common reasons women seek out hormone testing in perimenopause are hot flashes, low mood, weight gain, brain fog and decline in memory. Research shows these symptoms to be primarily symptoms of low oestrogen in the brain. Health care providers might consider symptoms of cognitive decline a good reason to test sex hormones. Testing sex hormones and monitoring symptoms during peri- and post menopause remains an effective way to assess oestrogen and oestrogen therapy’s long-term health for the brain and body. DUTCH testing shows not only the patient’s oestrogen levels but how they are metabolising oestrogen, which can be helpful in lowering the risks of hormones as in breast cancer.
What about Men? It appears that oestrogen benefits men’s neurological health, too. Although testosterone decline is common as men advance in age, men do continue to make testosterone throughout their natural life. Due to aromatisation, men typically have higher oestrogen in their later years than post-menopausal women. In healthy men who are not on hormones, there are no events of significant oestrogen decline equivalent to menopause in women. However, some older men do experience low testosterone, and possibly concurrently low oestrogen. This highlights the importance of testing men to make sure their oestrogen is in range (not too high or low). This may be particularly necessary if the men are on exogenous testosterone (which may get converted to oestrogen) or an aromatase inhibitor (which blocks oestrogen production).
References
Janicki, S.C. and N. Schupf, Hormonal influences on cognition and risk for Alzheimer’s disease. Curr Neurol Neurosci Rep, 2010. 10(5): p. 359-66.
Paganini-Hill, A. and V.W. Henderson, Estrogen deficiency and risk of Alzheimer’s disease in women. Am J Epidemiol, 1994. 140(3): p. 256-61.
Maki, P.M., et al., Perimenopausal use of hormone therapy is associated with enhanced memory and hippocampal function later in life. Brain Res, 2011. 1379: p. 232-43.
Resnick, S.M. and V.W. Henderson, Hormone therapy and risk of Alzheimer disease: a critical time. JAMA, 2002. 288(17): p. 2170-2.
Resnick, S.M. and V.W. Henderson, Hormone therapy and risk of Alzheimer disease: a critical time. JAMA, 2002. 288(17): p. 2170-2.
Janicki, S.C. and N. Schupf, Hormonal influences on cognition Maki, P.M., et al., Perimenopausal use of hormone therapy is associated with enhanced memory and hippocampal function later in life. Brain Res, 2011. 1379: p. 232-43.and risk for Alzheimer’s disease. Curr Neurol Neurosci Rep, 2010. 10(5): p. 359-66.
https://www.aihw.gov.au/reports/life-expectancy-death/deaths-in-australia/contents/leading-causes-of-death